Mind Mapper
Sun advances understanding of the brain networks that regulate behavior and mood
Research at Risk: Since World War II, universities have worked with the federal government to create an innovation ecosystem that has yielded life-changing progress. Now much of that work may be halted as funding is withdrawn. Find out more about the threats to medical, engineering, and scientific research, as well as how Harvard is fighting to preserve this work—and the University's core values.
Wendy Sun’s interest in neuroscience stems from her experience growing up in an immigrant family. Born in China, Sun moved to the United States with her parents when she was four years old, a transition that was challenging and stressful. She saw some of those close to her struggle with depression and anxiety.
“I think being an immigrant has taught me a lot of lessons in resilience and adapting to new environments,” she says. “I think in some ways, it can also make you vulnerable to anxiety and depression because of the amount of stress that you go through at an early stage in life. And in Chinese culture—particularly in the older generations—we don’t really talk about mental health. It’s kind of brushed off like, ‘Oh, you know, you can just work harder and you’ll be fine.’ That was pretty challenging for me growing up.”
A PhD student in medical sciences at the Harvard Kenneth C. Griffin Graduate School of Arts and Sciences, Sun advances understanding of how the brain organizes and executes complex behaviors, such as when we take action to achieve a goal. At the same time, as an MD candidate at Harvard Medical School, Sun brings her research to a clinical setting to better understand the workings of transcranial magnetic stimulation (TMS), a new treatment for obsessive-compulsive disorder (OCD), addiction, and depression.
Task Master
Sun studies the activity of specific brain regions and networks and measures their effects on behavior and mood. “The research question is, ‘How are advanced behaviors like decision making, forming goals and following them, planning for the future—basically anything that’s complex and requires thought—organized in the human brain?’” she says.
In recent years, it has become increasingly clear to neuroscientists that no single part of the brain supports complex behaviors. Instead, networks distributed across different regions of the brain serve different functions, sometimes sharing functions as well. The frontoparietal network, for instance, includes portions of the lateral prefrontal and posterior parietal cortexes, among other brain regions, and is thought to be involved in a wide variety of tasks.
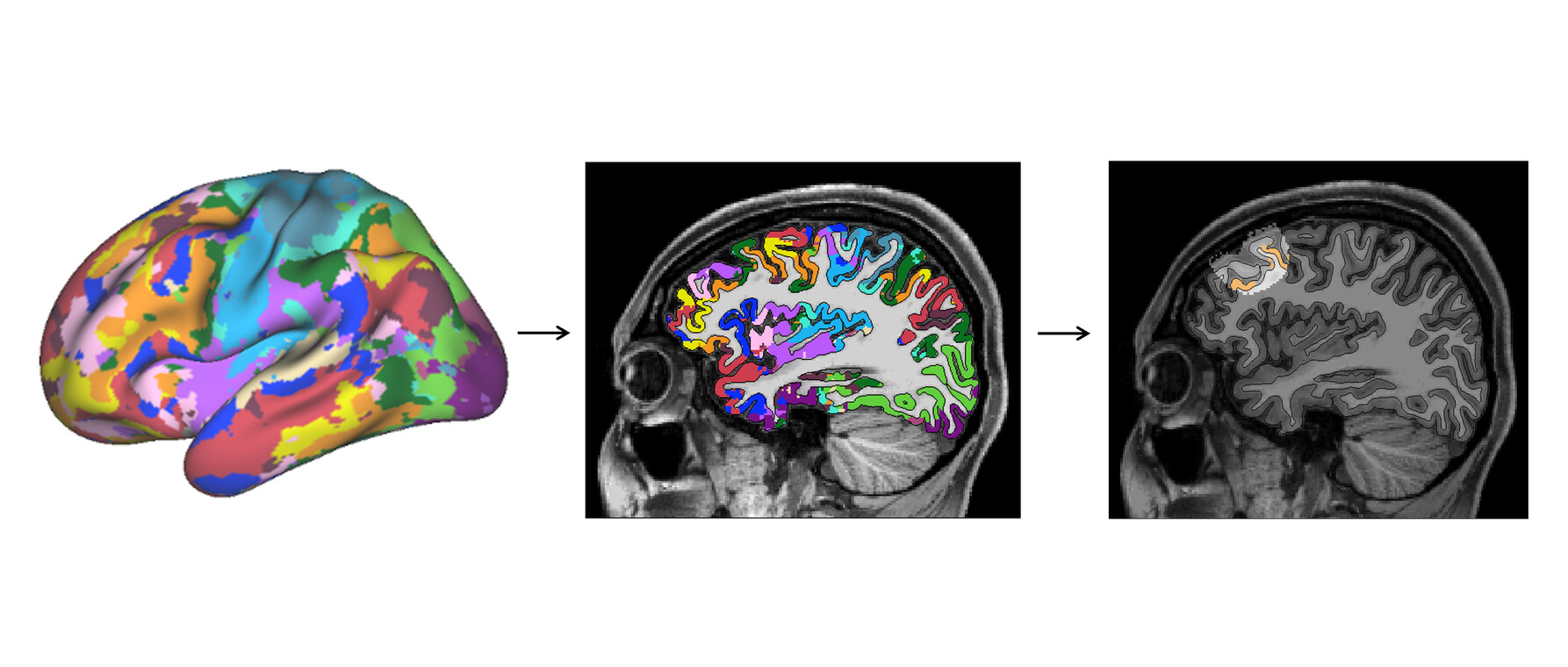
Sun and her colleagues leverage a method developed at the lab of Harvard Professor of Psychology and Neuroscience Randy Buckner to identify and target these networks in individual subjects using functional magnetic resonance imaging (fMRI), which measures brain activity by detecting changes in blood oxygen levels. “At Buckner lab, we recruit human subjects and put them in an MRI scanner,” Sun explains. “We ask them to do various tasks like remembering the past or imagining the future, and we scan the subjects very intensively over a course of several months using fMRI imaging to get a proxy of brain activity, measure, and characterize their neural networks.”
To identify and map the demanding mental process known as cognitive control—the ability to regulate thoughts and actions in response to goals and situations—Sun and her colleagues at Buckner lab have subjects participate in a task called the “N-back” game. She shows subjects a series of pictures or words on a screen and asks them to indicate if the current item matches the one they saw a certain number of turns before (in this case, zero or two). For example, if a subject sees a picture of a cat, they might be asked to remember whether it was the same image as the one they saw two turns before. Or they might be asked to remember if a word they’re presented with rhymes with the one they saw previously. “These tasks require holding in mind different rules and information and constantly updating them,” Sun says. “It’s pretty difficult for the brain to do.”
You can imagine that if we can measure these [neural] networks [involved in depression and OCD] and functionally characterize them, we can also manipulate them in a clinical sense.
—Wendy Sun
In efforts led by postdoctoral fellow Jingnan Du, Peter A. Angeli, Lauren M. DiNicola, Sun and her colleagues first identified patterns of spontaneous activity coupled together when people were in resting state—one in which there was little demand on their cognitive processes. Then they analyzed data from challenging tasks the individuals engaged in like the N-back game. They found they could identify when a particular network was preferentially activated in an individual’s brain. In all, they mapped 15 different networks.
“We found that the networks we identified during resting state—for example, the frontoparietal control networks—recapitulated themselves,” she says. “In other words, the tasks were engaging the networks that we identified in a totally independent set of data for the same individuals. It was real.”

Disruptive Innovation
Sun now turns to transcranial magnetic stimulation for the translational phase of her research. A noninvasive procedure, TMS involves placing an apparatus over a subject’s scalp and delivering brief magnetic pulses that induce electric currents in the underlying brain tissue. These currents can either increase or decrease the activity of neurons, depending on the frequency and intensity of the stimulation. Recently approved by the US Food and Drug Administration, TMS can be used to treat patients with psychiatric disease.
“Patients with conditions like OCD, addiction, and depression . . . the networks in their brains responsible for higher-order functions aren’t working properly,” Sun says. “You can imagine that if we can measure these networks and functionally characterize them, we can also manipulate them in a clinical sense. TMS pulses disrupt neural activity in the part of the brain that’s immediately close to the skull or the cortex, which is where these networks are thought to live.”
A safe and well-tolerated procedure, TMS has only minimal side effects like mild discomfort or headache. (Sun has tried the procedure herself and she says the sensation is “like being flicked with a rubber band.”) The only serious risk is seizure, which is rare and can be prevented by screening for those who are predisposed.
TMS has shown promise for patients with severe depression who do not respond well to other treatments such as antidepressants or psychotherapy. But much is still unknown about how the therapy works and how it can be optimized for different patients and conditions. “TMS as a treatment is constantly evolving,” says Professor Buckner, who serves as Sun’s faculty advisor. “Each person is different, and each brain is different. Wendy takes on the challenging task of asking why some approaches are more effective and why TMS works better for some individuals more than others.”
Wendy has been instrumental in designing outcome measures that will allow us to assess the effects of the treatment on specific changes in patients’ mood and behavior.
—Dr. Mark Eldaief
After identifying networks using fMRI, Sun plans to use TMS to stimulate different regions of the brain in both healthy controls and patients with depression to observe the effect on cognitive function. Dr. Mark Eldaief, a psychiatrist and neurologist at Massachusetts General Hospital and one of Sun’s mentors, says that although depressive symptoms vary widely, TMS is still applied in a “one-size-fits-all” manner. Eldaief says that Sun’s research could help make it possible to personalize treatment and target specific depressive symptoms.
“There is mounting evidence that dysfunction in specific networks gives rise to specific depressive symptoms,” he says. “Our laboratory hopes to use precision-based delineations of brain networks in the individual to identify network targets for TMS. Wendy has been instrumental in designing outcome measures that will allow us to assess the effects of the treatment on specific changes in patients’ mood and behavior. It’s no exaggeration to say that this project would not be able to move forward without Wendy’ s brilliance, determination, and good nature.”
Promising Future
Inspired by her immigrant experience—and with the support of a Paul and Daisy Soros Fellowship for New Americans—Sun continues to search for treatments that help people like those in her community who live with anxiety, depression, and other mental health issues. “Growing up in an immigrant family was formative for going to med school and researching these different systems in the brain and how we can treat them,” she says. “Just seeing people around me struggle with different kinds of psychiatric disease was very motivating.”
Now in the fifth year of her MD/PhD, which typically takes eight years to complete, Sun says she enjoys the program’s balance between research and clinical application. “They complement each other very well,” she says. “Being a clinician helps me ask better research questions, and being a researcher helps me understand the mechanisms behind the diseases that I see in patients.”
Excited about the future of neuroscience and its application in therapies like TMS, Sun hopes in the years to come to combine her clinical and research skills to develop new interventions for patients with mental health disorders.
“TMS is a very promising technique,” she says. “I think it’s very powerful because it can actually change brain activity in a causal way, not just observe it. And I think it can also be personalized to each individual’s brain anatomy and function. There’s a lot of room for improvement and optimization, but I think it’s already showing very impressive results.”





